Featured Experts: Nisha Aggarwal Gilotra, M.D.
Myocarditis occurs when the heart muscle becomes inflamed. When your heart muscle is inflamed, it can affect your heart’s electrical system. This can cause arrhythmia, or a rapid or abnormal heartbeat. Myocarditis can cause the heart muscle to weaken and can lead to cardiomyopathy.
Johns Hopkins cardiologist and heart failure expert Nisha Aggarwal Gilotra, M.D., explains symptoms, causes and treatment for myocarditis.
What is myocarditis?
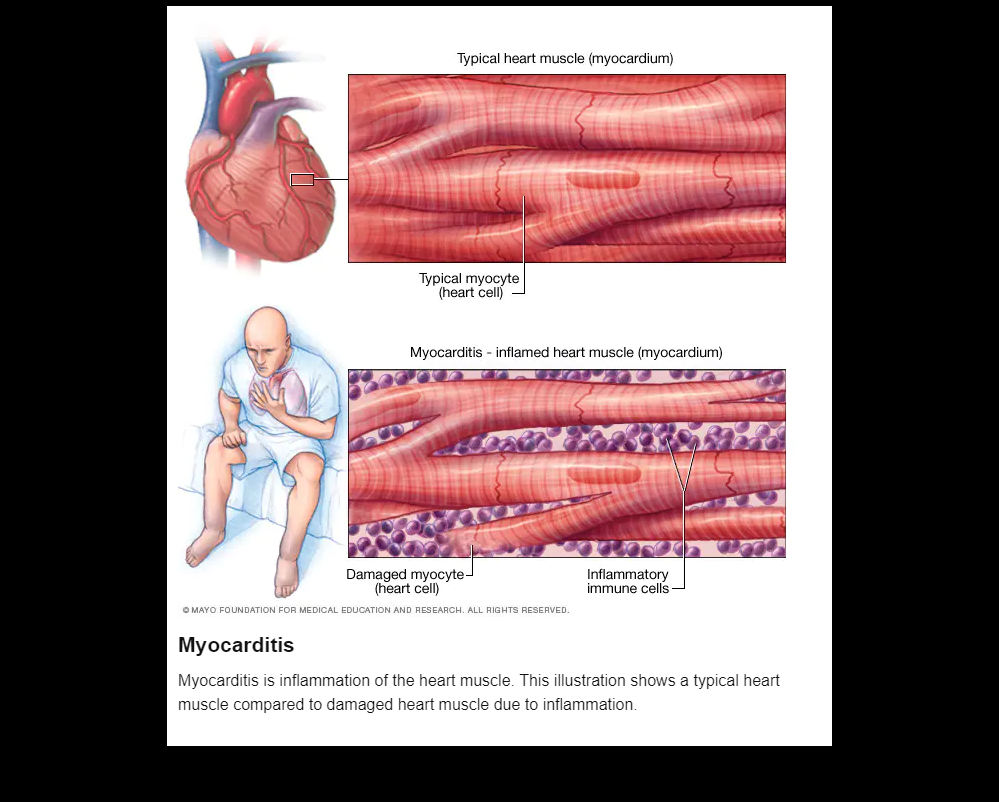
Myocarditis occurs when the heart muscle (myocardium) becomes inflamed. Inflammation occurs when your body’s immune system responds to infections, for example. Myocarditis can be caused by viral infections or more systemic inflammatory conditions such as autoimmune disorders. In severe cases of myocarditis, the heart muscle weakens and cannot pump blood effectively to other parts of your body.
There are several types of myocarditis; some examples include:
Acute myocarditis
Acute myocarditis describes relatively recent or fast onset of myocarditis and is usually caused by a viral infection. Acute myocarditis can develop suddenly, and symptoms may resolve rapidly as well.
Chronic myocarditis
Chronic myocarditis is when it takes longer than usual to treat the disease or when symptoms reappear after experiencing the condition. This can occur due to more general inflammatory conditions such as autoimmune disorders, in which your immune system attacks healthy cells and tissue in your body.
Lymphocytic myocarditis
Lymphocytic myocarditis is a rare form of myocarditis that can result in hospitalization for acute care. It occurs when white blood cells (lymphocytes) enter and cause inflammation of the heart muscle. This condition can occur after a virus.
Myocarditis Symptoms
In the early stage of myocarditis, you may have few or no symptoms at all. Common symptoms may include:
- Chest pain
- Fatigue
- Rapid or abnormal heart rhythm (arrhythmia)
- Signs of infection:
- Diarrhea
- Headache
- Fever
- Muscle aches
- Sore throat
- Shortness of breath
- Swelling in legs
Myocarditis Diagnosis
Myocarditis can be difficult to diagnose due to nonspecific symptoms and signs. Your doctor will ask for a thorough review of your medical history and symptoms, and may perform the following tests:
- Blood test
- Chest X-ray
- Electrocardiogram (ECG)
- Echocardiogram (ultrasound of the heart)
- Cardiac MRI or biopsy may be indicated in some cases.
Myocarditis Causes
Myocarditis is rare, but when it occurs, it is most commonly caused by an infection in the body. Infections from viruses (most common, including those that cause the common cold, influenza or COVID-19), bacteria, fungus or parasites can lead to myocardial inflammation.
Autoimmune diseases such as lupus, sarcoidosis and others can also cause myocarditis because the immune system can attack any organ in the body, including the heart, causing inflammation. Drugs or other environmental or toxic exposures can lead to myocarditis as well.
Myocarditis Treatment
There is no curative treatment for myocarditis. However, your doctor may treat an underlying cause of your myocarditis if identified, and may prescribe the following medications based on the cardiac symptoms (heart failure, arrhythmia), type of myocarditis and how severe it is:
- Angiotensin-converting enzyme (ACE) inhibitor / angiotensin receptor blockers (ARBs): Lower blood pressure and help with remodeling of the heart muscle after myocarditis.
- Beta blockers: Improve arrhythmias and help with remodeling of the heart muscle.
- Diuretics: Help decrease fluid congestion in the body, which can occur when the heart muscle weakens.
- Corticosteroids: Reduce inflammation in the body; reserved for specific causes of myocarditis.
In severe cases, where heart rhythm disorders occur, your doctor may implant a pacemaker or implantable cardioverter defibrillator (ICD). If the heart function does not improve and continues to cause severe heart failure, you may be evaluated for a heart transplant.
Your doctor may also recommend lifestyle changes, which may involve a low-salt diet and fluid restriction.
Myocarditis Recovery Time
Most cases of myocarditis are self-resolving. Other cases recover several months after you receive treatment. In some cases, this condition can recur and can cause symptoms related to inflammation such as chest pain or shortness of breath.
Original Article – https://www.hopkinsmedicine.org/health/conditions-and-diseases/myocarditis